Dr. Ernest W. Ramsey Manitoba Prostate Centre
The Dr. Ernest W. Ramsey Manitoba Prostate Centre at CancerCare Manitoba is the provincial centre for prostate disease. The centre provides timely access to diagnosis and therapy of both benign and malignant diseases of the prostate. You may be referred to the centre by your urologist or family physician for assessment and diagnosis by our health-care team.
Our multidisciplinary team of urologic surgeons, radiation oncologists, medical oncologists, nurses, a psychosocial clinician and registered dietitian offer assessment, diagnostics and treatment for men with prostate disease.
Patients and their families also receive education and supportive care, as well as co-ordinated access to additional resources as necessary.
If you are diagnosed with prostate disease, there are a number of treatments available and our team will help you to decide which is best for you.
Dr. Ernest W. Ramsey Manitoba Prostate Centre
ON3200 (3rd floor)
675 McDermot Ave
Winnipeg, Manitoba R3G 1C3
204-787-4461
Monday – Friday, 8 a.m. to 4:15 p.m.
Closed holidays
Prostate Disease Information
There are two main types of disorders associated with the prostate. These disorders include benign prostate diseases and prostate cancer. Benign prostate diseases include two conditions which are:
- prostatitis or inflammation of the prostate gland affects men of all ages
- benign prostatic hyperplasia (BHP) or enlargement of the prostate affects older men
The other main prostate disease is prostate cancer. Prostate cancer is a complex disease that is most commonly found in older men. Many risk factors have been associated with its development including race, age, genetics, lifestyle, etc.
For more information on any of the conditions listed above; please click on the associated disease or condition.

The prostate is a small gland about the size and shape of a chestnut. It is situated just below the bladder and surrounds the urethra, the passage that carries urine from the bladder through the penis during urination.
Women do not have a prostate.
The prostate secretes fluid, which forms part of the semen in which sperm are transported. During sexual activity and orgasm, the semen enters the urethra and passes along it through the penis to the outside. This is called ejaculation.
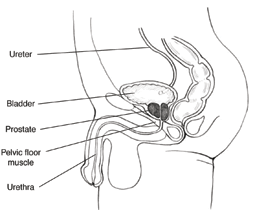
Most men notice that around age 50, they begin to experience some changes in their urinary functioning. This is caused by enlargement of the prostate gland which compresses the urethra, the tube which carries urine from the bladder to the outside. This is called benign (non cancerous) prostatic hyperplasia and is NOT cancer of the prostate.
Symptoms of prostate enlargement include:
- A sudden urgent need to urinate (urgency)
- An increase in the number of times you need to urinate during the day or night (frequency)
- A weak stream when you pass urine
- Not being able to urinate at all (retention)
- Straining when urinating
- Hesitation before the stream of urine begins to flow
- Feeling that the bladder has not emptied completely
- Dribbling or leakage of urine
- Pain when urinating
- Occasional blood in the urine (hematuria)
Diagnostic Tests
Depending on the symptoms, a variety of tests will be ordered to help in the diagnosis of BPH. These may include:
- A urine test to detect the presence of blood or infection.
- A blood test to check how your kidneys are functioning.
- An ultrasound of your abdomen to visualize the kidneys and bladder.
- Cystoscopy in which a small telescope is passed through the urethra and into the bladder. This causes a small amount of discomfort.
- Urine flow studies which help to identify if the symptoms are caused by a blockage in the urethra. To do this test you will urinate in the usual manner into a special container and the strength of the flow is recorded.
- Urodynamic studies in which urine flow and bladder volume and pressure are measured via a small catheter which is passed into the bladder via the urethra.
A measure of the residual volume of urine is left in your bladder after urinating normally. This can be measured by ultrasound over the bladder or by passing a catheter into the bladder and measuring how much urine remains in the bladder after urination.
Treatment Options
Treatment is usually offered based on how bad the symptoms are. Some men decide to live with their symptoms and not have treatment. Others opt for either medical or surgical treatment to alleviate symptoms.
Drug treatments
There are two types of drugs used to treat BPH:
- Alpha-blockers relax the muscles of the prostate and bladder neck and improve urination. Men usually notice an improvement in their symptoms within a few days or weeks of starting treatment but these benefits last only when taking the medication. Side effects include fatigue, dizziness, nasal congestion and retrograde ejaculation (ejaculate does not come out of the penis with orgasm but rather flows into the bladder).
- Five alpha-reductase inhibitors block testosterone and reduce the size of the prostate thereby decreasing pressure on the urethra. It may take several months to see reduction in symptoms and you have to continue to take these medications over the long term because if you stop, the prostate will just enlarge again. Side effects include loss of libido, erectile dysfunction and decrease in the amount of ejaculate.
- A combination of these two treatments is highly effective but may result in an increased risk of side effects.
Surgical treatments
Another highly effective treatment of BPH is the surgical removal of prostate tissue where it is compressing the urethra. Transurethral resection of the prostate (TURP) is usually done by passing an instrument through the urethra and removing tissue from inside the prostate gland. Some urologists use a laser to remove the tissue. In some instances, the urologist needs to make an incision in the abdomen to gain access to the prostate gland; this is called an open prostatectomy.
Side effects of the surgery include retrograde ejaculation (semen passes into the bladder during orgasm instead of to the outside of the body). Some men may experience loss of erectile functioning after the procedure however this is rare.
Most men will experience a marked improvement in their urinary symptoms following this procedure however some will need a repeat of the surgery years later if symptoms recur.
Prostatitis is an extremely frustrating disease because the correct diagnosis of your problem is difficult and it cannot always be cured. However, prostatitis is a treatable disease and you can usually get some relief from you symptoms by following the recommended treatment.
The bacteria that cause acute and chronic bacterial prostatitis get into the prostate from the urethra by backward flow of infected urine into the prostate. Bacterial prostatitis is not contagious and is not considered to be a sexually transmitted disease. If you have a diagnosis of bacterial prostatitis, your sexual partner cannot catch this infection from you.
Certain conditions or medical procedures increase the risk of contracting bacterial prostatitis. You are at higher risk for getting prostatitis if you:
- recently have had a urinary catheter or other instrument inserted into your urethra
- have an abnormality of your urinary tract
- have had a recent bladder infection
Non-bacterial prostatitis or prostatodynia (now called chronic pelvic pain syndrome) may not be due to the typical bacteria that cause urine infections. It maybe caused by one of the following reasons:
- organisms called Chlamydia or mycoplasma or even organisms that cannot be cultured using standard techniques
- urine itself flowing backwards into the prostate ducts,
- immune (or allergic) problems
- repetitive trauma to the perineal area (for example from a bicycle seat)
- a problem with the nerves and muscles surrounding the prostate gland (longer term cases)
Prostatitis is categorized into four separate categories:
The symptoms of the various prostatitis syndromes are extremely variable and although they depend on the type of disease you have, there is considerable overlap.
Category I
Acute bacterial prostatitis is caused by bacteria and is treated with antibiotics. Acute bacterial prostatitis comes on suddenly and with a severity that may warrant you seeking medical help immediately. Symptoms are severe and include:
- pain
- chills
- fever
- sever burning when attempting to urinate
- voiding problems (e.g. inability to empty your bladder)
Category II
Chronic bacterial prostatitis is also caused by bacteria and requires antibiotics. Unlike an acute infection, symptoms of chronic bacterial prostatitis may be less severe but are still extremely distressing, particularly during a flare-up and can include:
- burning on urination
- urinary frequency
- frequent urination at night
- perineal, testicular, bladder and/or low back pain
- painful ejaculation
- prostate is swollen and tender during examination by physician
Recurrences are common and you may have no symptoms between episodes
Category III
Chronic pelvic pain syndrome (non-bacterial prostatitis or prostatodynia) is not caused by the usual bacteria and its cause is unknown. Antibiotics may not be effective for this type of prostatitis but will be considered by your physician because of the difficulty in differentiating bacterial from non-bacterial prostatitis. The symptoms of non-bacterial prostatitis and prostatodynia (Category III chronic pelvic pain syndrome) can be indistinguishable from those of chronic bacterial prostatitis and may also include the following common symptoms:
- discomfort or pain in the area of the perineum, bladder area, testicles, prostate and/or penis
- voiding difficulties are common (e.g. urination)
- frequent urination
- painful urination
- Difficult and/or painful ejaculation is also a very common complaint
Category IV
Asymptomatic prostatic inflammation is diagnosed on biopsy and does not usually require treatment.
What other disease cause similar symptoms?
- Benign prostatic hyperplasia (BHP) is a non-cancerous enlargement of the prostate gland that is very common in men over age 50 and may produce urinary tract symptoms that are similar to those experienced with prostatitis.
- Urethritis, an inflammation of the urethra (usually caused by a bacterial or sexually transmitted organism), may also give rise to many of the symptoms that one experiences with prostatitis. Similarly, cystitis or infection of the bladder produces similar symptoms.
- Prostate cancer, which occurs in the same age group as BPH, can cause discomfort and voiding symptoms that can be mistaken for prostatitis.
Prostate cancer occurs when the cells of the prostate begin to grow uncontrollably. When caught and treated early, prostate cancer has a cure rate of over 90%. Prostate cancer is the most common cancer diagnosed in men and the risk for this cancer increases with age.
We do not know the cause of prostate cancer. We do know that the prostate requires the male hormone testosterone for its development and that prostate cancer is also partly dependent on testosterone for its growth.
Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the life of the man diagnosed, but also the lives of his family members in significant ways for many years to come.
Prostate Cancer Information
Symptoms of Prostate Cancer
In its early stages, prostate cancer does not produce symptoms.
As it enlarges, it compresses the urethra interfering with normal urination and may produce symptoms which include the following:
- Frequent urination
- Weak urinary stream
- Incontinence (loss of urinary control)
- Painful urination
- Blood in urine
Cancer that has spread to bone, then pain may occur, most commonly in the back and hips.
Prostate Cancer by Stage
Staging determines the extent of prostate cancer and include the three following stages.
- Localized prostate cancer means that the cancer is confined to the prostate.
- Locally advanced prostate cancer means that most of the cancer is confined within the prostate, but some has started to escape to the immediate surrounding tissues.
- In metastatic disease, the prostate cancer is growing outside the prostate and its immediate area, possibly to more distant organs.
A number of tests can be used to determine the stage of disease. Locally advanced prostate cancer is most frequently detected through traditional imaging studies, such as CT scans and x-rays, or through bone scans.
Cancers that spread to more distant organs tend to travel through the lymphatic system.
Knowing the stage of disease can help to determine how aggressively the disease needs to be treated, and how likely it is to be eradicated by the available treatment options.
Diagnostic Tests
To help make an accurate diagnosis your physician will utilize the following examinations:
Digital Rectal Examination (DRE)
Since the prostate is located just in front of the rectum, your doctor can feel it by inserting a lubricated gloved finger into the rectum. This is called a digital rectal examination (DRE). The presence of lumps or hardness within the prostate will suggest prostate cancer. Not all lumps in the prostate are cancerous and a biopsy will be done to confirm or exclude cancer. A DRE is performed in men presenting with symptoms of difficulty with urination. A DRE may also be performed during a general medical examination to try and detect the cancer before symptoms occur.
The PSA Blood Test
PSA is a protein produced by the prostate and released in very small amounts into the bloodstream. When there's a problem with the prostate, such as when prostate cancer develops and grows, more and more PSA is released, until it reaches a level where it can be easily detected in the blood.
To measure PSA, a small amount of blood is drawn, and the level of PSA is measured. PSA levels under 4 ng/mL are usually considered "normal," however, depending on the age of the man, what is considered normal may be lower than that.
PSA can also be elevated if BPH or prostatis are present and some men with prostate cancer have "low" levels of PSA. This is why both the PSA and DRE are used to screen for the presence of disease and an abnormal result usually leads to a more accurate test, the prostate biopsy.
Biopsy
During a biopsy, a needle is inserted into the prostate to take 12 to 14 small samples of tissue under the guidance of ultrasound imaging called transrectal ultrasound (TRUS).
TRUS is not a test to screen for prostate cancer. It is performed in patients suspected of having cancer based on DRE or PSA. TRUS produces an image of the prostate and permits accurate placement of the biopsy needle into selected areas of the prostate. It is performed by inserting a probe just slightly larger than the index finger into the rectum.
The biopsy procedure may cause some discomfort, however it is performed under local anaesthesia and most men do not report that it is painful. The samples are sent to the laboratory where they are examined by the pathologist where the sample is graded and scored (see Gleason Grading and Gleason Scores for more detailed information).
Gleason Grading and Gleason Scores
Normal prostate cells, just like all other cells in the body, are constantly reproducing and dying, and each new prostate cell has the same shape and appearance as all of the other prostate cells. But cancer cells look different, and the degree to which they look different from normal cells is what determines the cancer grade. "Low-grade" tumor cells tend to look very similar to normal cells, whereas "high-grade" tumor cells have changed so much that they often barely resemble the normal cells.
The Gleason grading system accounts for the five distinct patterns that prostate tumor cells tend to go through as they change from normal cells. The scale runs from 1 to 5, where 1 represents cells that are very nearly normal, and 5 represents cells that don't look much like prostate cells at all.
After examining the cells under a microscope, the pathologist looking at the biopsy sample assigns one Gleason grade to the most common pattern in that sample, and a second Gleason grade to the next most common pattern. This is repeated for each of the samples taken from the prostate gland. The two grades are added, and the Gleason score, or sum, is determined for that sample.
Generally speaking, the Gleason score tends to predict the aggressiveness of the disease and how it will behave. The higher the Gleason score, the less the cells behave like normal cells, and the more aggressive the tumor tends to be.
If the biopsy shows cancer then other tests may be done to check if it has spread including.
- A bone scan involves injection of a radioisotope, which can demonstrate metastases to bone.
- A CT scan is a special type of x-ray sometimes is done to assess spread to lymph nodes.
Treatment Options
There is no "one size fits all" treatment for prostate cancer. It is important to learn about the various treatment options and, in conjunction with the health care team, make a decision about the best option. For most, the decision will rest on a combination of clinical and emotional factors. Men diagnosed with localized prostate cancer today will likely live for many years, so any decision that is made now will likely have an influence on him and his family for a long time.
Careful weighing of the various options (listed below) is an important first step in deciding on the best treatment course.
Active Surveillance
The concept of active surveillance is a viable option for men who, for one reason or another, have decided not to undergo immediate surgery or radiation therapy.
During active surveillance, the cancer is carefully monitored for signs of progression. A PSA blood test and DRE are usually administered every three to six months along with repeated biopsies of the prostate. If tests indicate that the cancer is growing, treatment is usually initiated.
Active surveillance might be a good choice for men who have very slow growing or very early cancers, or for men who have other serious medical conditions that are likely to shorten their lifespan.
Also, many of the treatment options for prostate cancer have significant side effects, and better outcomes are seen in men who are otherwise healthy. If a man has been diagnosed with other disorders or diseases, such as heart disease, long-standing high blood pressure, or poorly controlled diabetes, his doctors might feel that it is in his best interest to hold off on surgery and avoid its potential complications.
Radical Prostatectomy (Surgery)
A surgical approach toward the treatment of prostate cancer can be used to remove the prostate gland and seminal vesicles. Typically, men with early-stage disease or cancer that is confined to the prostate will undergo radical prostatectomy.
In this surgery an incision is made in the abdomen and the prostate is cut out. This is called an open prostatectomy. Wherever possible, the surgeon attempts to avoid cutting the erectile nerves that run alongside the prostate.
After removing the prostate, the surgeon stitches the urethra directly to the bladder. To allow internal healing to take place, the surgeon inserts a catheter into the bladder. With this in place, urine flows into a bag. The catheter is usually kept in place for about 10 to 14 days.
Some surgeons are able to do this surgery using sophisticated instruments called laparoscopes. In laparoscopic surgery, very small incisions are made in the abdomen, into which the surgeon inserts narrow instruments fitted with cameras and/or surgical tools, allowing the surgeon to visualize and operate on the internal structures without making a larger incision in the abdomen.
Side Effects of Surgery
The side effects of this surgery include incontinence (leakage of urine) as well as erectile dysfunction.
Incontinence
In the immediate period after the catheter is removed, most men will be unable to control the flow of urine. This is very distressing and many men feel hopeless when this occurs. There tends to be fairly rapid improvement of this immediate incontinence and most men manage with one or two pads a day for the first few months. As time passes, they gain more control and this is assisted if they do pelvic floor exercises on a regular basis. The nursing staff will give you instructions on how to do these exercises. There are also continence experts who can provide you with additional training and treatment using biofeedback. If you are interested in seeing a continence expert, ask the nurse for a referral.
Erectile dysfunction
Immediately after surgery for prostate cancer almost all men will be unable to have an erection. Erections may return over the following weeks, months or even years. Return of erections depends on what your erections were like before surgery, your age, your general health and lifestyle factors, and the amount of damage to the nerves.
Many men will have erectile problems after surgery. You may not have any erections at all, they may not be hard enough for penetration, and they may not last long enough to satisfy either you or your partner. Many men also notice that the penis is both shorter and smaller in girth than before. This results from both the surgery and shrinkage of tissue in the period following surgery when there is reduced blood flow to the penis due to lack of erections.
There are a number of oral medications that can be taken that may help you have an erection. These medications prevent blood from leaving the penis once it has entered the tissues following physical stimulation of the penis. This is the least invasive method of treating erectile difficulties and is usually the first treatment that your doctor will suggest. More invasive treatments include the vacuum pump, the intra-urethral pellet (MUSE™) and penile self-injection therapy.
There is some suggestion that taking oral medication to help get erections can increase the likelihood that spontaneous erections will return earlier after surgery. The Manitoba Prostate Centre offers a program for penile rehabilitation; you can ask your urologist about this.
The Clinical Nurse Specialist at the Manitoba Prostate Centre can help you with sexual problems. She can be reached at 787-4495 and a physician referral is not necessary.
Radiation Therapy
Radiation involves the killing of cancer cells in the prostate gland with directed radiation. There are two types of radiation therapy used to treat prostate cancer.
External Beam Radiation Therapy
The most common type of radiation therapy is external beam radiotherapy. CT scans are used to map out the location of the prostate gland, and the radiation is targeted directly at this area. Using 3D conformal radiotherapy, a computerized program maps out the exact location of the prostate gland so that the highest dose of radiation can reach the cancer cells within the gland.
Treatment is given five days a week for about seven or eight weeks in the Radiation Therapy Department of CancerCare Manitoba.
Brachytherapy ("seeds")
With brachytherapy, tiny metal pellets (they look like small pieces of pencil lead) containing radioactive iodine are inserted into the prostate via needles that enter through the skin of the perineum (behind the scrotum). Careful and precise maps are used to ensure that the seeds are placed in the proper locations. This is a day procedure which is performed under general anaesthetic and men go home a few hours after.
Over the course of several months, the seeds give off radiation to the immediate surrounding area, killing the prostate cancer cells. By the end of the year, the radioactive material degrades, and the seeds are inactive.
Side effects of radiation therapy
Men who have been treated with radiation tend to experience irritation of adjacent tissue from the radiation and this may affect bladder and bowel functioning.
Men may need to urinate more frequently and may experience some burning pain when they pass urine.
They may also have some diarrhea.
These side effects tend to improve in the days and weeks following the end of treatment.
Radiation therapy also poses a risk to erections although this tends to occur one to two years after treatment is completed and is much more gradual than the changes noticed after surgery. The same treatments used for erectile dysfunction after surgery can be tried by men after radiation therapy.
Androgen Deprivation Therapy (Hormone Therapy)
Prostate cancer cells need testosterone to grow and survive. To starve the cancer of this hormone, androgen-deprivation therapy or ADT, is designed to stop testosterone from being released or to prevent the hormone from acting on the prostate cells. ADT is most often used for men with more advanced prostate cancer or in addition to radiation therapy. It may also be used if the cancer recurs after treatment.
The majority of cells in prostate cancer respond to the removal of testosterone. But some cells grow independent of testosterone, and therefore remain unaffected by androgen deprivation therapy. As these hormone-independent cells continue to grow unchecked, over time, androgen deprivation therapies have less and less of an effect on the growth of the cancer.
While androgen deprivation therapy does not cure the disease, it remains an important step in the process of managing advancing disease.
The most common types of androgen deprivation therapies are described below. Although each of these therapeutic options is effective at controlling prostate cancer growth, the loss of testosterone causes significant side effects in nearly all men.
Orchiectomy
Because about 90% of testosterone is produced by the testicles, surgical removal of the testicles, or orchiectomy, is an effective solution to blocking testosterone release. This approach has been used successfully since the 1940s, but is not commonly performed since the development of medical treatments.
For men who choose this option, the procedure is typically done on an outpatient basis in the urologist's office. Recovery is rapid and no other treatment is needed.
Luteinizing-hormone releasing hormone (LHRH) Agonists
Luteinizing-hormone releasing hormone, is one of the key hormones released by the body which prompts the testicles to produce testosterone. (Note that LHRH is sometimes called GnRH, or gonadotropin-releasing hormone.) Blocking the release of LHRH through the use of LHRH agonists or LHRH analogues is one of the most common hormone therapies used in men with prostate cancer. This shuts down the body's release of testosterone.
Drugs in this class, including leuprolide (Eligard, Lupron), goserelin (Zoladex) are given in the form of regular injections.
Anti-androgens
LHRH agonists cause what is known as a "flare" reaction because of an initial transient rise in testosterone in response to the altered signals to produce testosterone. This can result in a variety of symptoms ranging from bone pain to urinary frequency or difficulty.
Anti-androgens are medications which help to block the action of testosterone in prostate cancer cells. They are therefore often added to the LHRH agonist for the first 4 weeks of therapy when the flare reaction typically occurs. In this setting, anti-androgens can be helpful in preventing the flare reaction.
Side effects of these treatments include the following:
- hot flashes
- fatigue
- loss of energy
- loss of libido (sexual desire)
- erectile dysfunction
Some men experience weight gain, hair loss and difficulties with memory and concentration. Long term use can also increase the risk of osteoporosis and men are encouraged to increase their calcium intake and exercise regularly. If osteoporosis does occur, there are treatments to prevent bone fractures which your physician will discuss with you.
Other Treatment Options
Surgery and radiation therapy remain the standard treatment for localized prostate cancer, but other, less popular treatment options might be beneficial as well. As time goes on and the benefits of these treatment options are further explored, it's possible that they will move more into the mainstream. For now, though, none are seen as standard treatments for localized prostate cancer.
Cryotherapy
Cryotherapy, also known as cryosurgery or cryoablation, uses freezing to destroy the prostate cancer. With this approach, probes are inserted into the prostate through the perineum (the space between the scrotum and the anus), and argon gas or liquid nitrogen is delivered to the prostate, literally freezing to death the prostate cells and any prostate cancer.
The freezing may affect both urinary and erectile functioning and side effects tend to be quite common.
High-Intensity Focused Ultrasound (HIFU)
High-intensity focused ultrasound works in the opposite way to cryotherapy: with HIFU, the prostate cells are heated until they die. A probe is inserted into the rectum, from which very high-intensity ultrasound waves are delivered to the target area. Although this technique remains experimental in the Canada, it's been used in Europe for a number of years with a fair amount of success.
HIFU is not available at the Manitoba Prostate Centre.
It’s through research that we gain new knowledge in the treatment of prostate disease and the effects of this disease on men and their families.
There are two main types of disorders associated with the prostate. These disorders include benign prostate diseases and prostate cancer.
Benign prostate diseases include two conditions:
- prostatitis or inflammation of the prostate glandaffects men of all ages;
- benign prostatic hyperplasia or enlargement of the prostateaffects older men.
The other main prostate disease is prostate cancer, which is a complex disease most commonly found in older men. Many risk factors have been associated with its development, including race, age, genetics, lifestyle, etc.
At some time, you may be asked if you would be interested in participating in different kinds of studies. Your permission is required to participate and you do not have to take part.
Recruitment and eligibility to participate in clinical trials taking place at the Manitoba Prostate Centre/CancerCare Manitoba may change. It’s best to ask about trials that you may be eligible for during a physician visit.

